Make advance medical decisions for conditions including terminal illness, permanent coma, Alzheimer’s, and pregnancy.
You have options when making advance health care decisions. Depending on your state’s laws, you can request different treatments for different situations. Most states allow you to make medical directives covering what you want if you are permanently unconscious or near death from a terminal illness, but some states let you cover other situations, too. This article explains the scenarios you might want to think about when planning ahead, so you can stay in control of decision making in health care even if you can’t communicate. We also discuss how pregnancy might affect the wishes you include in your medical directive.
Close to Death From a Terminal Condition
A terminal condition usually means a disease or injury that doctors believe cannot be cured and is likely to cause death soon, such as advanced cancer. State laws may define terminal conditions slightly differently, but they often use terms like "incurable" or "hopeless." In many states, terminally ill patients would not survive without artificial life support. Most states require one or two doctors to confirm a terminal condition before following your health care instructions, and some require this confirmation in writing.
Doctors often state that people with a terminal illness have fewer than six months to live. Many people in this situation choose comfort care, using medication and IVs to manage pain and avoiding surgeries or tests. However, some people live longer than expected. If you decide against life-prolonging treatment, remember you are taking a risk that your condition will not improve, so consider your choices carefully.
Permanently Unconscious
Permanent unconsciousness can result from medical conditions, head trauma, or body injuries and is sometimes called a persistent vegetative state (PVS) or permanent coma. Permanently unconscious people appear to have sleep cycles and respond to some stimuli, though experts debate whether they experience pain. Most don’t need mechanical breathing or circulation support but require food and water through feeding tubes.
It can be hard to diagnose permanent unconsciousness because the signs are not always clear, and mistakes can happen. Sometimes, things like too much medication can look like permanent unconsciousness but get better with different treatment. To avoid mistakes, many states require two doctors, including a specialist, to confirm the diagnosis before following advance directives. Your health care agent can help by making sure the diagnosis is correct and getting a second opinion if needed.
Once a condition is diagnosed as permanent, the chance of recovery is very small. Still, medical technology can keep someone alive for a long time. Allowing a natural death may mean stopping tube feeding and fluids. There is no single right answer about what to choose in this situation; your own values about quality of life should guide you. Some people want all treatments in case a cure is found. Others feel life without awareness is not worth living and refuse all treatments, even food and water. Many choose a middle ground, like accepting feeding tubes but not other life support.
If you find this decision difficult, talk to a doctor or health care professional you trust. You can also look for online resources that discuss the medical, spiritual, and personal aspects of these choices.
Additional Medical Conditions
Some states have laws for situations where death is not imminent, but the condition cannot be reversed. If your state covers one of these situations, you can decide what treatment you want. The table below lists these conditions by state.
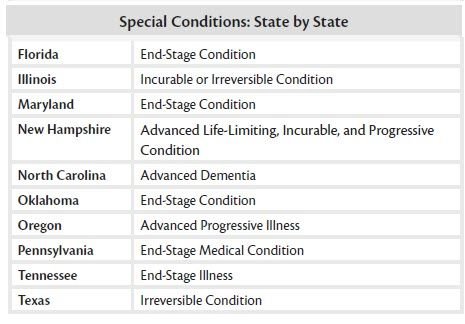
If The Burdens Outweigh the Benefits
In addition to the conditions above, you can give your health care agent the power to withhold or stop treatments that are not in your best interest. (Oregon does not allow this.) If you do not name an agent, this power, if you allow it, goes to your legally appointed surrogate, usually a spouse or close family member.
This instruction applies only if you refuse life-prolonging treatment or artificially administered nutrition and hydration in all other cases. It lets your decision maker stop treatments in situations not covered by your state’s rules, like late-stage Alzheimer’s disease, which may not count as "terminal" or "permanently unconscious."
Your wishes are important in deciding what is in your "best interest." Some states say your wishes are final, while others involve doctors in the decision. Including this in your advance directive orders makes your decision maker’s role clear and can help prevent disagreements.
Giving this power means your decision maker will have significant control over your care. Talk with your agent and loved ones about which benefits or burdens matter most to you. For example, would having to leave your home for hospital care be a big enough burden for you to refuse life-prolonging treatment?
How Pregnancy May Affect Your Wishes
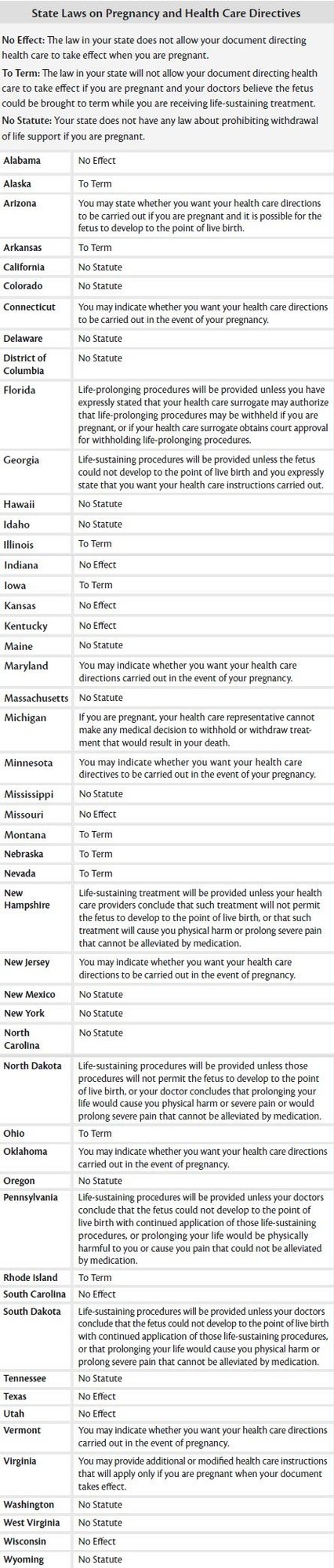
Pregnancy presents a unique circumstance where your advance health care instructions may face legal obstacles. In many states, laws prohibit medical providers from withdrawing or withholding life-sustaining treatment from pregnant individuals—or require such treatment to continue if the fetus could potentially survive to birth.
These state limitations have drawn criticism from reproductive rights advocates. For decades, such restrictions faced legal challenges based on U.S. Supreme Court precedents establishing constitutional protections for reproductive autonomy. The Supreme Court's recent reversal of federal abortion protections has intensified debates over mandatory life support for pregnant individuals, even when it conflicts with their expressed wishes.
Because this issue is controversial and hospitals or family members may have different opinions, it is important to clearly document your preferences. If you can become pregnant, you should state whether you want your health care instructions to be:
- suspended during pregnancy, or
- enforced regardless of pregnancy status.
If you choose to suspend your directives during pregnancy, medical providers will decide what care is appropriate. In most cases, they will give all available life-sustaining treatments, especially if the fetus is four to five months along and seems healthy and able to survive.
If you decide to keep your health care instructions in place during pregnancy, be ready for possible resistance from medical providers. This is more likely if your directives limit life-sustaining treatment, nutrition and hydration, or comfort care.
Resistance usually grows as pregnancy continues. In the second trimester (months four to six), doctors will likely provide all treatments they think are needed to protect both your life and the fetus. In the third trimester, it may be almost impossible to get around state rules that require life-sustaining care.
If you feel strongly about challenging your state’s restrictions, meaning you live in a state that cancels your directive during pregnancy but you want it followed, talk in detail with your health care agent and prepare them to advocate for you. You may also want to include a detailed explanation of your wishes in your health care directive.
Who Decides What Kind of Care You'll Get?
You may be wondering who will make decisions about your medical care if your medical condition keeps you from being able to speak for yourself. If you've named an agent in your advance directive or medical power of attorney, that person will tell medical professionals what you would want based on instructions you've provided or their best understanding of your wishes.
If you haven't named an agent, medical staff will look to close family for decision-making -- usually a spouse, child, sibling, etc. Most states have established a specific hierarchy of decision-makers for this situation.
Of course, in emergencies, there isn't time for medical professionals to consult your agent or your advance directive, and those medical providers will have to make the best decisions they can in the moment. To help them, consider making a POLST and/or DNR, discussed next.
Emergencies, POLSTs, and DNRs
- medical power of attorney -- to name an agent to speak for them
- a medical directive -- to detail what kind of care they want
- a DNR -- to keep in their medical record to inform caregivers not to perform life-saving measures, and
- a POST -- to put on display for emergency medical personnel.
More Information About Advance Health Care Planning
Making an advance health care plan that fits your medical choices and concerns helps make sure your values guide your treatment if you cannot speak for yourself. By planning ahead for these situations, you give your loved ones and medical providers clear guidance for the future.
For more information, see the following articles:
- Writing a Final Wishes Document
- Advance Health Care Planning: Specifying Your Wishes
- Expressing Organ Donation Wishes in Your Health Care Directive
You can learn more about making health care directives valid in your state in WillMaker’s Legal Manual.